There have been two maternal deaths here in the past two weeks. There have been just as many near misses. There are women at the hospital right now whom might soon fall into either of the above categories. There have been several sets of twins born, several normal births, many cesareans. Being an observer at this Haitian hospital, where Midwives For Haiti students are practicing their clinical skills, is an ongoing juxtaposition of tragedy and hope.
I’ve watched Midwives For Haiti students take vitals and chart progress. I’ve seen them dance with their patients to help the baby down and lovingly rub their backs during hard contractions. I watched a student catch a baby and then later do a full newborn exam.
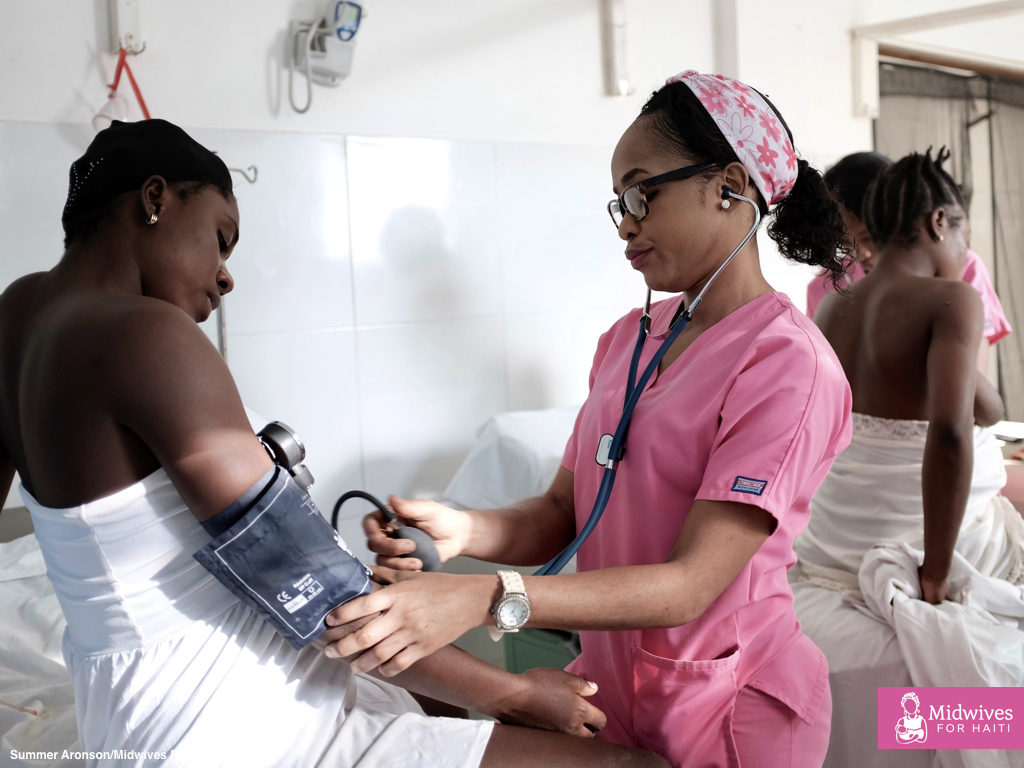
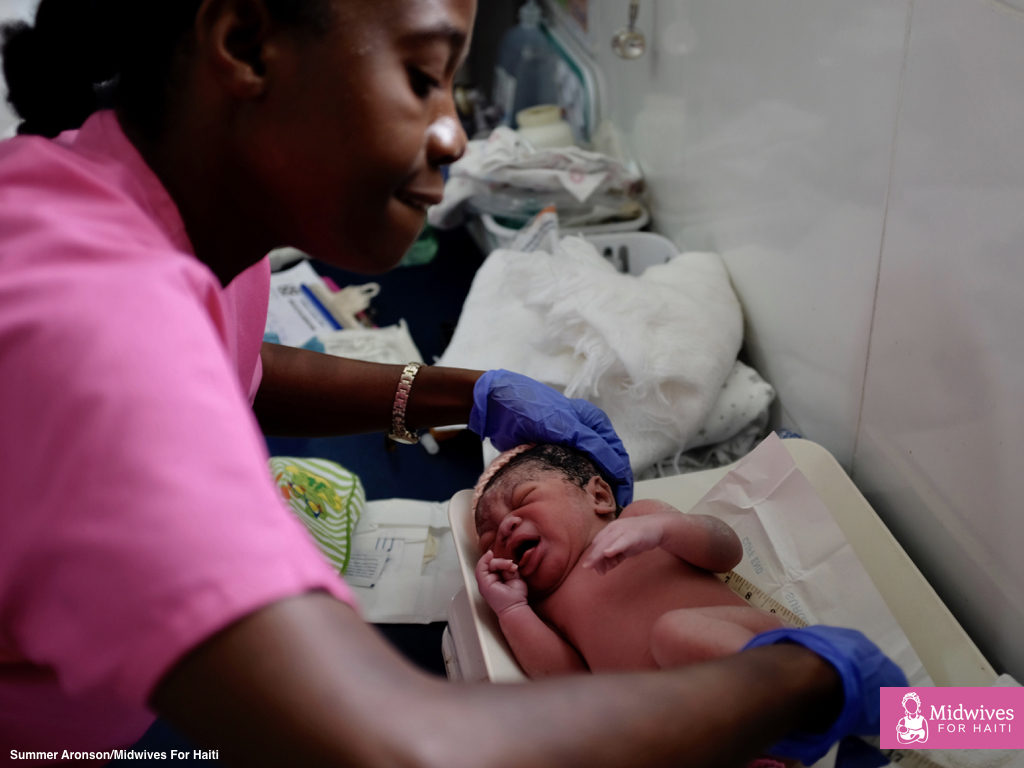
I also observed a crisis.
On a busy morning, a mother was brought into the hospital: 24 weeks pregnant, dark red blood in her urine, and blood pressure of 240/130 (a normal BP is 120/70). At first, the students could find heart tones for the baby, then they couldn’t. The baby died as the staff struggled to find a vein for mom’s IV.
Mom was conscious, but barely. Her family member was holding her IV bag as the staff worked. The last time I looked at her, she was vomiting. Within a few hours, she had a seizure: eclampsia, the leading cause of maternal death in Haiti and nearly always preventable. Mom was moved to ICU.

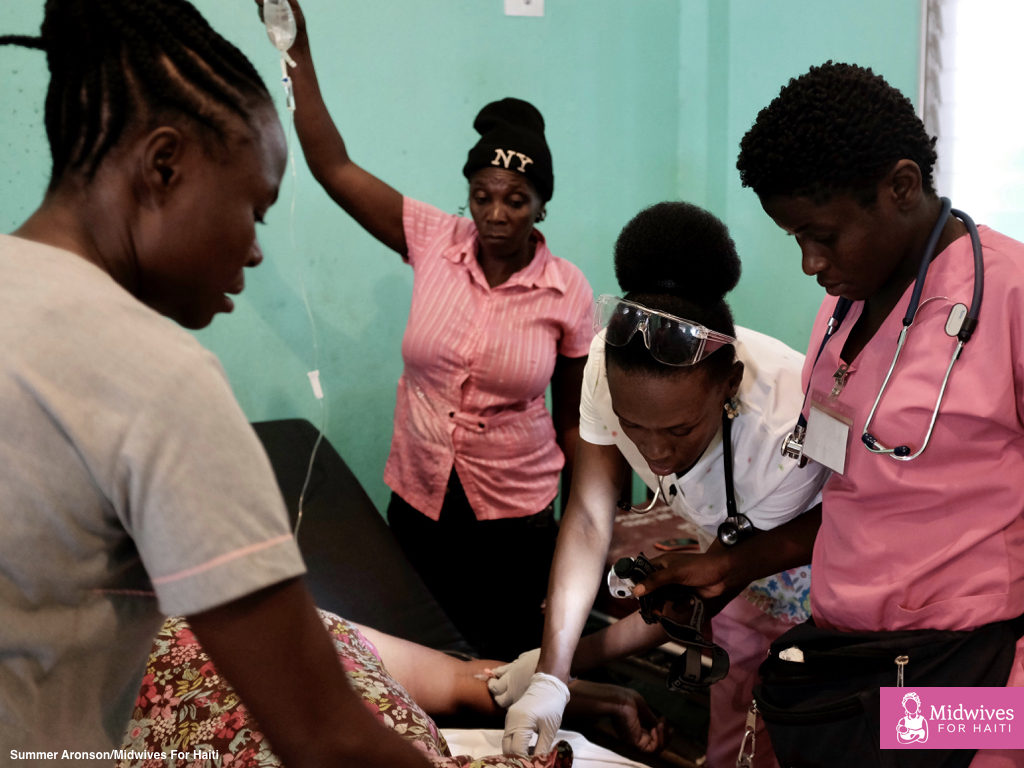
The next day, our Clinical Director, Perrine, reported that they were still unable to bring her blood pressure down. Perrine stayed with her all day. At 8pm that night, during a tropical downpour, we receive a frantic call from Perrine needing help. Two midwives jump into their scrubs and grab towels to cover themselves from the rain. No motos will come because of the rain and a car finally arrives. When they arrive at the hospital twenty minutes later, Perrine is doing chest compressions on the mom. There is no defibrillator at the hospital and the doctors present are struggling to perform CPR correctly. Perrine is on her own. She brings two fists down hard on mom’s chest, trying to shock her heart. It was the last best attempt. It was not enough.
In the postpartum wards, mothers lie on the sheets they brought from home with buckets next to the cot for their bodily waste. Some have babies with them, some don’t.
One mother lies very still. Her husband sits next to her with an anguished expression. There is no baby. This father and their family carried mom for twenty hours on a homemade stretcher to reach a car to take them the last of the way to the hospital. Mom, 28 weeks pregnant, was having seizures. Eclampsia, again. This mom survived, but she will never be the same. There is significant damage to her brain and her husband is beginning to realize this.
Last week, an 18 year old mother traveled over an hour and a half to reach the hospital. She was 31 weeks pregnant and hypertensive (high blood pressure and possible sign of preeclampsia, which leads to eclampsia). The baby was born alive by cesarean and then taken to the NICU. The following day, the young mother complained that she couldn’t breathe, a possible complication of the cesarean. Volunteer midwives discovered her oxygen saturation rate was 76%. She was moved to ICU and the volunteers consulted with a resident doctor. They agreed to pay the $50 USD for the oxygen she needed, otherwise she would go without and most certainly die.
By the next day, the young mother is better. She still has not received any news about her much loved baby, was it a boy or girl? Was it okay? The volunteer midwives go to the NICU to find out. You have a baby boy, they tell her, and there was a crisis and he is not doing well. Tears pour from her eyes and she is soon sobbing.
Permission is received from the NICU nurses to have mom come into the NICU. She must stand near the door and they hold up her son to see. She knows her baby is dying. She comes back again later and sits near him for 40 minutes. It is as close as she will get to his breathing body.
This mother has no one with her to care for her so she is not eating. Our staff buys her dinner. The next day they tell this young mom that her baby has passed away. She is so sad. But she is also stuck here now. The hospital, under new leadership, recently changed the policy and services are no longer free. This is a public referral hospital for one of the poorest regions of the poorest country in the Western Hemisphere. This means that many very high risk women, with few resources, come from far distances to receive life-saving care. But, now it comes with a price tag: vaginal births are 500 goudes ($10 USD) and cesareans are 5000 goudes ($90 USD). Women are not allowed to leave until they pay. We have no control of this policy and, in my opinion, it is criminal. How these families find the money is a mystery but I am told that someone will go back to their community and sell an animal or borrow money from multiple relatives.

This bereaved young woman, who lives an hour and a half away, is all alone. She has no one to raise the money for her. And she is afraid the hospital will come looking for her if she leaves. Our staff assure her that she lives far enough away and she’ll be safe. They give her some money for a moto to take her home. Go quickly, they say, just go. And she does.
These are just a few stories in the span of 10 days in Haiti. The crises do not stop when I leave. I hear from Perrine that there have already been several more “difficult cases” since I left just a few days ago. It is heart wrenching. If these moms had access to adequate prenatal care and education, there is a good chance these stories would have very different endings. It is why I have so much hope for Midwives For Haiti students and graduates –about 20% of the skilled maternity workers in Haiti– who fan out all over Haiti, providing care to tens of thousands of women each year.
On that night the rain poured from the heavens and a mother was lost, the wailing of her grieving family haunted the hospital. They had first grieved the baby, now they lost the mother, too. She was their daughter, sister, aunt, and wife. It was her first baby and she was in her late twenties, the same age when I had my first child. I will never forget seeing this young woman surrounded by midwives and students, her eyes closed and the slight shaking of her head “No” before slipping unconscious.
In Haiti, being pregnant is often not a joyous experience. It is scary. We discuss this reality over dinner with a visiting journalist who mentions once spending time in a war torn hospital in the Middle East. He described how victims of war would be carried in and the bright white hospital floors were pooled in blood. That happens here, too. In Haiti, childbirth is a woman’s war.
And we’re fighting. But, it’s hard.
Fight with us. Your support makes a difference. Click here to help us raise $75,000 by Dec 31 and win extra cash prizes.
– Summer Aronson
Communications & Marketing Director, Midwives For Haiti
November 9, 2017
–
If you’d like to purchase a defibrillator for our use in Haiti, please email info@midwivesforhaiti.org. Thank you.

